Microdosing with GLP-1 medications is popping up increasingly in online communities, but it has no official standing in proven clinical guidelines. The idea sounds very appealing — fewer side effects, more control — but it lacks scientific backing.
Yet more and more people are experimenting with lower doses or adjusted intervals of semaglutide and tirzepatide, often without medical supervision. That raises questions about safety, effectiveness, and what you can realistically expect when you deviate from standard dosing.
The 5 Key Takeaways
- There is no approved protocol for microdosing — what you read online is experimental and not evidence-based
- Lower doses can reduce side effects, but may also weaken the effect on weight and blood sugar
- Active concentration builds up due to the long half-life of GLP-1 medications
- Compounding pharmacies offer flexibility, but quality and purity vary significantly
- Nausea and stomach complaints are often temporary — stopping or lowering isn’t always necessary
What is GLP-1 microdosing?
In pharmacology, microdosing refers to a dose far below the therapeutic threshold, intended to study pharmacokinetics without clinical effect. With GLP-1 medications, the term is used more loosely: any dose lower than the standard starting dose of 2.5 mg tirzepatide or 0.25 mg semaglutide is quickly labeled ‘microdosing.’
That’s actually imprecise. Research from UCLA Health shows that even official starting doses are titration phases designed to limit side effects, not true microdosing. Real therapeutic effects on weight usually only occur at 5 mg tirzepatide or 1 mg semaglutide, so anything below that could be called subtherapeutic.
Pros and cons: what does science say now?
The advantage of lower doses lies mainly in reduced gastrointestinal complaints like nausea, vomiting, and constipation. Some people report less extreme appetite suppression, allowing them to stick to a healthy eating pattern without extreme hunger suppression.
The downside is that you’ll likely lose weight more slowly or take longer to achieve blood sugar control. Verywell Health emphasizes that there are no clinical trials supporting the safety or effectiveness of self-designed microdosing schedules. You mainly risk uncertainty and disappointment.
Pros and cons of GLP-1 microdosing
Advantages
- Lower risk of nausea and vomiting during the first weeks
- Gradual adjustment to reduced appetite
- Dosing flexibility when using compounding vials
- Lower cost per injection with lower doses
Disadvantages
- No official guidelines or clinical evidence for safety
- Possibly insufficient effect on weight or HbA1c
- Trial-and-error can take weeks or months
- Risk of underdosing when independently splitting prefilled pens
Example of gradual titration and practical considerations
The official titration schedules for tirzepatide and semaglutide increase by one step every four weeks, for example from 2.5 to 5 mg. Those experiencing side effects can consider delaying the increase, or adjusting the frequency — for example every five days instead of every seven. Medicijngebruik.nl explains that tirzepatide’s half-life is approximately five days, so more frequent doses lead to more stable levels.
What’s important is understanding that doses accumulate. After four injections, you reach a ‘steady state’ — the concentration still fluctuates, but stays within a range. If you take 2.5 mg weekly, at any given moment you have between 3.5 and 7 mg in your body, depending on when it’s measured.
Common mistakes and safety (compounding, needles, storage)
Many people switch to compounding pharmacies for more flexible dosing and lower costs. However, quality can vary significantly: some batches use research-grade peptides without pharmaceutical control. DokterTamara.nl warns of contamination, incorrect concentrations, and lack of sterility.
Additionally, storage mistakes are common — GLP-1 medications must be refrigerated before first use — and needle reuse, which increases infection risk. A missed dose can usually still be made up if within 48 hours; after that, you skip that week and resume your normal schedule.
Reducing side effects without losing results
Nausea and stomach complaints typically peak in the first 48 hours after injection and gradually decline afterward. NTvL emphasizes that most gastrointestinal effects are temporary — your body usually adjusts within two to four weeks. Lowering too early may just prolong this adjustment period.
Those still experiencing symptoms can opt for smaller, more frequent meals, adequate hydration, and fiber against constipation from delayed gastric emptying. Some doctors recommend temporarily taking a low-dose motility agent, but that requires individualization and medical consultation.
Glossary
- Half-life: The time it takes for a substance’s concentration in the blood to halve; approximately 5 days for tirzepatide, 7 days for semaglutide
- Steady state: An equilibrium condition in which the supply and breakdown of a medication are equal; reached after 4–5 half-lives
- Titration: Gradually increasing the dose to limit side effects and build efficacy
- Compounding: Preparation of medications by specialized pharmacies, often custom-made or cheaper than brand products
Who may benefit from lower doses?
According to experts, microdosing may be useful for maintenance after reaching target weight or stable HbA1c values. At that point, you no longer need maximum GLP-1 activity and may be able to get by with a lower, stable dose to prevent relapse.
For people with severe diabetes or significant obesity, a subtherapeutic dose seems less suitable. They typically need higher doses — sometimes 10 or 15 mg tirzepatide — to optimize insulin production and strengthen glucagon suppression. Trial-and-error with doses that are too low only delays reaching treatment goals.
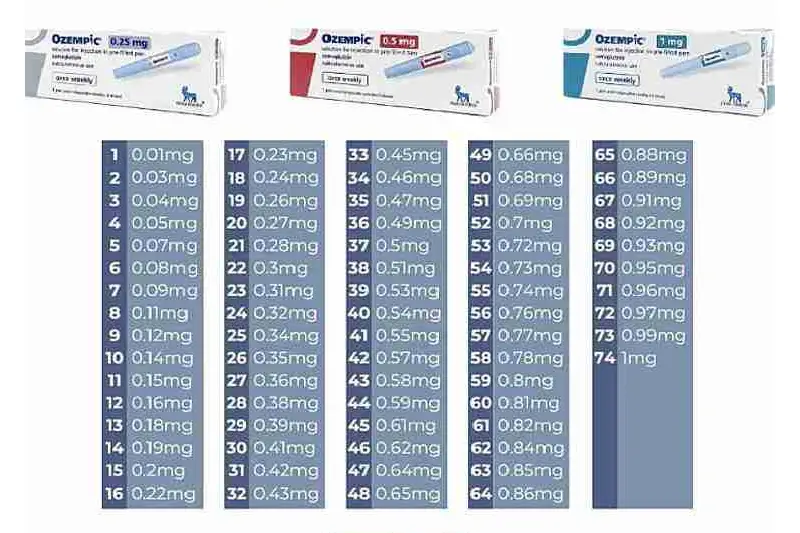
Practical overview: standard dosing and variations
| Medication | Starting dose (official) | Therapeutic dose (weight loss) |
|---|---|---|
| Tirzepatide | 2.5 mg/week | 5–15 mg/week |
| Semaglutide | 0.25 mg/week | 1–2.4 mg/week |
| Liraglutide | 0.6 mg/day | 1.8–3 mg/day |
Drug interactions and absorption issues
Due to delayed gastric emptying, blood levels of oral medications can fluctuate. Thyroid hormone (levothyroxine) and birth control are known examples where absorption decreases, leading to unintended pregnancies in some women. Consulting a doctor is essential if you use multiple medications.
Timing of administration also plays a role. Some medications — like iron supplements or certain antibiotics — are better taken with sufficient spacing to prevent absorption interference. A pharmacist or healthcare provider can recommend an adjusted dosing schedule.
Conclusion
Microdosing sounds appealing because it promises fewer side effects while maintaining effect, but that combination hasn’t been scientifically proven. What is established is that lower doses are less likely to lead to weight loss or blood sugar control.
Those who experiment anyway are best doing so under medical supervision, paying attention to compounding quality, injection hygiene, and realistic expectations. Trial-and-error is part of it, but don’t forget that official titration schedules exist for a reason — they balance effectiveness and safety based on clinical data, something self-designed microdosing protocols simply lack.
Verified Sources
- UCLA Health – GLP-1 microdosing is experimental and unauthorized – A framework piece emphasizing that no official guidelines or evidence-based schedules exist.
- Verywell Health – Is ‘Microdosing’ Ozempic Safe? – Overview of trend, safety concerns, and lack of clinical evidence.
- Medicijngebruik.nl – GLP1 agonists – Dutch-language basic information on mechanism and common side effects.
- DokterTamara.nl – Frequently asked questions about GLP-1 medication – Practical Q&A about side effects and what to expect in the first weeks.
- NTvL – Pros and cons of GLP-1 receptor agonists – Summary of long-term observations and possible additional effects.
Related Articles
Frequently asked questions
What exactly is GLP-1 microdosing?
Microdosing means deliberately using smaller-than-standard doses or more gradual increases of GLP-1 agonists to promote adjustment and limit side effects. It’s not an official guideline and falls outside registered dosing.
Is microdosing Ozempic or other GLP-1 medications safe?
Currently, there is no hard clinical evidence that microdosing is safe or effective; major institutions describe it as experimental. Always discuss with your doctor and preferably follow registered schedules.
What dosing schedule is often mentioned for microdosing?
In practice, schedules circulate with lower starting doses and slower titration (e.g., half-step increases), but these are not standardized and should, if considered at all, be strictly medically supervised.
What are the most common side effects and how do you limit them?
Common complaints include nausea, vomiting, diarrhea or constipation, reduced appetite, and abdominal pain. Slow titration, eating small portions, and limiting alcohol often help; with severe symptoms, always contact a doctor.
Can you take GLP-1 daily for microdosing or what do you do with a missed dose?
The registered administration is usually weekly; daily administration deviates from the product information. With a missed dose: usually resume according to label or doctor’s advice; after multiple missed doses, downward adjustment may be needed.




















I’ve been exploring cannabis terpene recently, and I’m deep down enjoying the experience. The scents are with, normal, and pleasant. They stretch a leaving caress to my broad daylight after age habit, ration congeal the delighted and atmosphere. A brobdingnagian bat upon for of anyone who appreciates severe wellness tools.